
Healthcare leaders across the globe face relentless pressure to control rising costs while improving outcomes. Traditional approaches no longer deliver sustainable results. Healthcare data analytics now drives a fundamental shift in how payers approach financial and operational strategies. Organisations increasingly rely on healthcare payer analytics to align cost, quality, and risk.
Global hospitals and insurers now prioritise healthcare digital transformation to build resilient systems. They leverage payer analytics solutions to uncover inefficiencies and act on real-time insights. This transformation enables smarter healthcare cost management and supports long-term value creation.
The Rise of Healthcare Payer Analytics as a Core Strategy for Cost Control
From Retrospective Reporting to Real-Time Healthcare Data Analytics
Healthcare organisations no longer depend on static reports. Modern systems use healthcare data analytics to deliver real-time insights. Decision-makers track cost trends instantly and respond faster to financial risks.
Why Global Hospitals and Clinics Depend on Data-Driven Payers
Hospitals and clinics now expect payers to contribute strategic insights. Strong payer-provider collaboration ensures shared accountability. Providers gain visibility into utilisation patterns, while payers improve cost forecasting.
Aligning Finance, Care, and Operations with Healthcare Analytics Tools
Organisations integrate finance, clinical, and operational data through healthcare analytics tools. This integration strengthens payer data management and enables seamless healthcare data integration across systems.
Decoding Healthcare Costs with Healthcare Data Analytics
Identifying Hidden Cost Drivers Across Data Sources
Payers analyse claims, clinical, and behavioural data using claims analytics in healthcare. These insights reveal inefficiencies such as unnecessary admissions and duplicate services.
Beyond Medical Loss Ratios with Healthcare Payer Analytics
Traditional metrics fail to capture full cost dynamics. Healthcare payer analytics provides deeper visibility into utilisation patterns and patient journeys.
How Healthcare Analytics Tools Enable Longitudinal Cost Analysis
Advanced platforms track patient costs over time. These tools support improving patient outcomes analytics by linking care quality with spending patterns.
| Metric | Without Analytics | With Analytics | % Improvement |
| Hospital Readmission Rate | 18% | 11% | 39% |
| Fraud Detection Accuracy | 65% | 92% | 41% |
| Claims Processing Time (Days) | 12 | 5 | 58% |
| Administrative Costs (% of Spend) | 25% | 18% | 28% |
This data highlights how healthcare data analytics significantly improves efficiency and cost control. Organisations reduce readmissions and administrative expenses while increasing fraud detection accuracy. Faster claims processing improves operational performance and customer satisfaction. These improvements directly support healthcare cost reduction strategies and demonstrate the value of payer analytics solutions in modern healthcare systems.
Source: McKinsey & Company – “The Potential of Healthcare Analytics to Reduce Costs”
Why Conventional Cost Management Models Fail Without Healthcare Analytics Tools
Challenges of Reactive Cost Containment
Traditional approaches to healthcare cost management rely heavily on retrospective analysis, which limits the ability to act in real time. These methods identify issues only after costs escalate, leaving little room for prevention. Without the support of advanced healthcare analytics tools, organisations struggle to detect inefficiencies early. In contrast, modern healthcare data analytics enables proactive monitoring, allowing payers to intervene before unnecessary expenses occur and optimise financial outcomes effectively.
Limitations of Network Restrictions and Prior Authorisation
Conventional strategies such as network restrictions and prior authorisation often focus on limiting access rather than addressing underlying inefficiencies. These methods fail to uncover patterns of misuse or systemic issues. Healthcare fraud detection analytics provides a more targeted and intelligent approach by identifying anomalies and suspicious behaviours in real time, ensuring better cost control without compromising patient access or care quality.
Replacing Assumptions with Evidence-Based Decisions
Data-driven organisations rely on healthcare data analytics to eliminate guesswork and improve accuracy in decision-making. Strong payer data management frameworks ensure that insights remain consistent, reliable, and actionable. Continuous monitoring, combined with integrated analytics, allows payers to refine strategies, enhance operational efficiency, and build sustainable cost control models.
Also Read – Why NLP Is The Missing Link In Data –Driven Hospital Management – Ezovion.
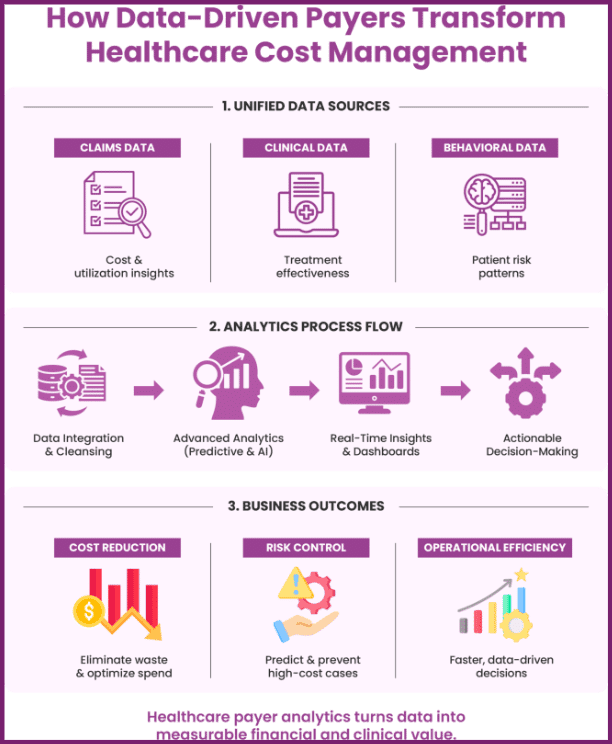
Leveraging Healthcare Data Analytics for Proactive Cost Optimisation
• Predictive Analytics in Healthcare Payer Analytics
Predictive models identify high-risk patients early. Risk adjustment analytics helps payers allocate resources efficiently.
• Reducing Avoidable Costs Through Risk Stratification
Payers use claims analytics in healthcare to identify preventable events. These insights reduce unnecessary hospitalisations.
• Real-Time Insights with Healthcare Analytics Tools
Modern healthcare analytics tools provide real-time dashboards. Teams act quickly and improve cost outcomes.
Transforming Risk Control with Healthcare Payer Analytics
From Static Risk Scores to Dynamic Models
Traditional scoring systems limit adaptability and fail to reflect real-time patient conditions. Risk adjustment analytics enables dynamic modelling by continuously analysing clinical, behavioural, and claims data. These advanced models respond to changing patient profiles, allowing payers to proactively manage high-risk populations. With the support of healthcare payer analytics, organisations gain deeper visibility into risk patterns and improve decision-making accuracy.
Supporting Value-Based Care Through Healthcare Data Analytics
Value-based care requires precise and timely insights. Healthcare data analytics empowers payers to align reimbursement models with actual patient outcomes. By integrating data across systems, organisations ensure that care quality and financial performance move in the same direction.
Balancing Financial Risk and Patient Outcomes
Payers achieve equilibrium by leveraging improving patient outcomes analytics alongside strategic cost allocation. This approach strengthens risk control while ensuring better care delivery.
Connecting Cost Efficiency to Outcomes with Healthcare Analytics Tools
• Population Health Analytics for Global Strategies
Population-level insights enable proactive interventions. Payer-provider collaboration strengthens care delivery.
• Closing Care Gaps While Controlling Costs
Healthcare payer analytics identifies gaps in care delivery. Organisations reduce long-term costs by addressing these gaps early.
• Improving Outcomes Through Data-Driven Decisions
Healthcare systems rely on improving patient outcomes analytics to enhance quality while reducing costs
| Investment Area | Average ROI (%) | Time to Value (Months) |
| Predictive Analytics | 150% | 12 |
| Fraud Detection Systems | 200% | 9 |
| Claims Automation | 120% | 6 |
| Data Integration Platforms | 130% | 10 |
Organisations that invest in payer analytics solutions achieve significant financial returns. Fraud detection delivers the highest ROI due to reduced losses. Predictive analytics improves care planning and reduces avoidable costs. Data integration enhances efficiency and supports better decision-making. These results reinforce the importance of healthcare digital transformation and show how analytics drives both cost savings and operational excellence.
Source: Deloitte – “Healthcare Analytics Adoption and ROI Report”

Building a Unified Ecosystem with Healthcare Data Analytics and Analytics Tools
Integrating Claims, Clinical, and Operational Data
Effective healthcare data integration eliminates silos. Organisations unify multiple data streams for better insights.
Role of Interoperability in Healthcare Payer Analytics
Interoperability enables seamless communication across systems. Strong payer-provider collaboration depends on integrated data.
AI and Machine Learning in Healthcare Analytics Tools
AI enhances healthcare fraud detection analytics and predictive modelling. It improves efficiency and accuracy across workflows.
Also Read – The Future Of Hospital IT – Interoperability As The Cornerstone Of Healthcare Innovation – Ezovion.
Transforming Risk Control with Healthcare Payer Analytics
• From Static Risk Scores to Dynamic Models
Traditional scoring systems restrict adaptability and fail to capture real-time clinical complexity. Modern risk adjustment analytics transforms this approach by enabling dynamic, continuously evolving models that process clinical, behavioural, and operational data streams. These models leverage healthcare data analytics to identify emerging risk patterns early and allow payers to intervene before conditions escalate. With advanced healthcare payer analytics, organisations improve risk stratification accuracy and optimise care pathways. This shift enhances population health management while supporting more precise resource allocation and proactive decision-making across payer ecosystems.
• Supporting Value-Based Care Through Healthcare Data Analytics
Value-based care depends on timely, data-driven insights. Healthcare data analytics allows payers to connect reimbursement with measurable patient outcomes. Through strong healthcare data integration, organisations unify fragmented datasets and create a comprehensive view of patient journeys. This alignment strengthens payer-provider collaboration, ensuring that financial incentives directly support quality care delivery.
• Balancing Financial Risk and Patient Outcomes
Payers achieve sustainable balance by combining improving patient outcomes analytics with strategic financial planning. This approach ensures effective risk mitigation while maintaining high-quality, outcome-driven care delivery.
The Future of Cost Management with Healthcare Data Analytics and Healthcare Payer Analytics
Healthcare organisations must embrace healthcare data analytics to remain competitive. Data-driven strategies improve cost control, risk management, and patient outcomes. Healthcare payer analytics empowers organisations to move from reactive cost containment to proactive cost intelligence.
Investment in payer analytics solutions and healthcare analytics tools will define the next phase of innovation. Organisations that prioritise healthcare cost reduction strategies and advanced analytics will lead the future of global healthcare.
Transform Your Cost Strategy with Advanced Healthcare Analytics Tools
Modern healthcare demands smarter strategies. Organisations must adopt healthcare data analytics, strengthen payer-provider collaboration, and invest in scalable technologies. These steps will unlock sustainable cost savings and improved outcomes.





