
Hospitals today operate under immense pressure. Clinical teams manage rising patient volumes, complex documentation requirements, and fragmented systems. Despite technological advancements, many healthcare organisations still struggle with healthcare workflow optimisation. Leaders now recognise that inefficiencies silently drain productivity, increase costs, and compromise patient outcomes.
The “workflow gap” reflects the disconnect between designed processes and real-world execution. This gap leads to lost clinical hours, delayed decisions, and reduced care quality. Effective hospital workflow management now demands intelligent systems that eliminate inefficiencies rather than amplify them.
What is the Workflow Gap in Healthcare Workflow Optimisation?
The workflow gap represents the difference between how hospital processes should function and how they actually operate. Clinical workflows often include multiple handoffs, approvals, and documentation steps. However, real-world execution introduces delays, duplication, and miscommunication.
Healthcare organisations frequently depend on disconnected systems that fail to support interdisciplinary workflow healthcare. Teams struggle to coordinate effectively, and clinicians spend excessive time navigating systems instead of delivering care. Without robust care team coordination systems, hospitals fail to achieve true efficiency.
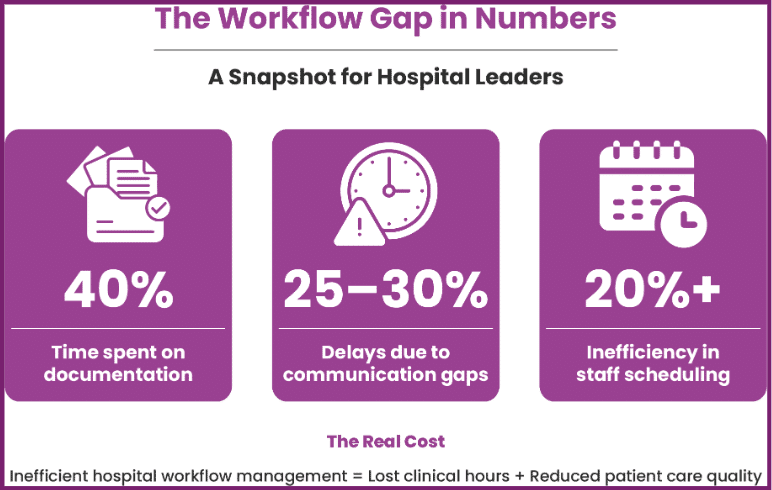
Where Workflow Gaps Occur in Hospital Workflow Management
Administrative Bottlenecks in Healthcare Workflow Optimisation
Administrative overload remains one of the biggest contributors to workflow gaps. Clinicians spend a large portion of their time on documentation and compliance tasks. Research shows that documentation alone can consume up to 40% of healthcare workers’ time, often exceeding time spent on direct patient care .
Doctor–Nurse Communication Breakdowns and Doctor Nurse Communication Tools
Poor communication disrupts care continuity. Many hospitals still rely on outdated systems instead of modern doctor nurse communication tools. Without effective care team coordination systems, delays occur in treatment decisions, handovers, and patient monitoring.
Inefficient Scheduling and Resource Allocation
Manual scheduling creates mismatches between staff availability and patient demand. Hospitals fail to leverage healthcare workflow automation, which leads to overworked teams and underutilised resources.
Fragmented Digital Systems
Multiple systems operate in silos, preventing seamless data exchange. This fragmentation weakens interdisciplinary workflow healthcare and forces clinicians to switch between platforms repeatedly.
The 5 Major Reasons Behind Workflow Gaps in Hospital Workflow Management
• Over-Reliance on Manual Processes
Manual workflows slow operations and introduce errors. Hospitals that ignore healthcare workflow automation continue to lose valuable time.
• Lack of Integrated Hospital Workflow Management Systems
Disconnected platforms prevent seamless data flow and hinder decision-making.
• Poor Data Visibility and Delayed Decisions
Leaders struggle to access real-time insights without integrated dashboards.
• High Administrative Burden on Clinicians
Studies show documentation tasks significantly increase workload and contribute to burnout .
• Resistance to Digital Transformation
Hospitals that resist innovation fail to adopt AI workflow assistant healthcare solutions that streamline operations.
Also Read – AI Vs Chaos: How Intelligent HIMS Platforms Are Redefining Emergency Care – Ezovion.
The Real Impact: How Workflow Gaps Affect Patient Care
Workflow inefficiencies directly affect patient outcomes. Hospitals lose valuable time that clinicians could spend on care delivery.
| Impact Area | Observed Effect | Operational Outcome |
| Documentation Overload | Up to 40% time spent on documentation | Reduced patient interaction |
| Nurse Workload | Up to 41% time on documentation | Increased fatigue |
| Physician Documentation | Increase from 16% to 28% post-EHR | Lower efficiency |
| Communication Delays | Fragmented workflows | Slower decision-making |
Hospitals that fail to implement care team coordination systems struggle to deliver timely care. Poor doctor nurse communication tools worsen coordination gaps and increase the risk of clinical errors.
Why Traditional Hospital Workflow Management Approaches Fail
Traditional systems focus on digitisation rather than optimisation. Hospitals implement electronic records but fail to redesign workflows. As a result, clinicians experience increased documentation time instead of reduced workload. Research indicates that electronic systems can initially increase documentation time for physicians by 17.5% . Without proper design, digital tools create additional friction rather than efficiency. Hospitals must move beyond basic digitisation and adopt AI healthcare workflow optimisation strategies.
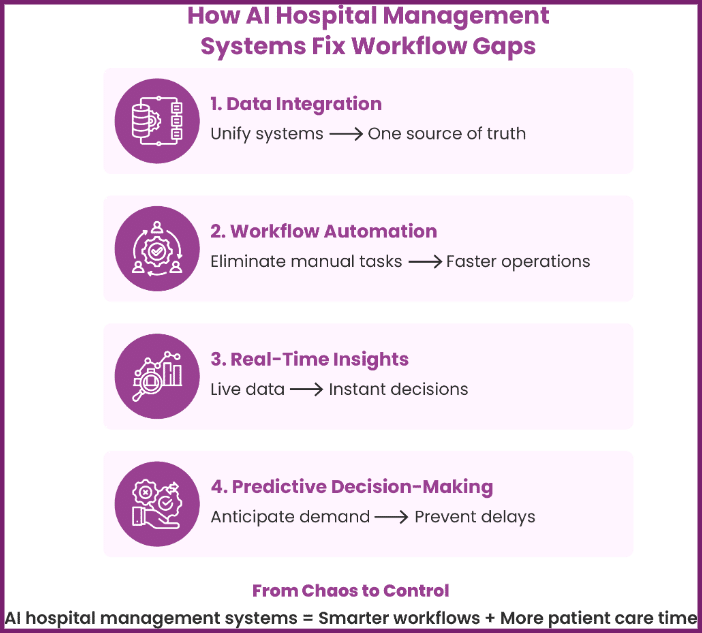
AI Healthcare Workflow Optimisation: Closing the Workflow Gap
AI healthcare workflow optimisation introduces intelligence into hospital operations. AI systems analyse data, automate tasks, and provide real-time insights.
Key capabilities include:
- Automation of repetitive tasks through healthcare workflow automation
- Predictive analytics for resource allocation
- Smart alerts and decision support
- Enhanced interdisciplinary workflow healthcare coordination
AI enables hospitals to move from reactive processes to proactive decision-making.
How AI Healthcare Workflow Optimisation Eliminates Workflow Gaps
• Intelligent Scheduling and Resource Allocation
AI predicts patient inflow and allocates staff accordingly. Hospitals optimise workforce utilisation using AI workflow assistant healthcare tools.
• Automated Clinical Documentation
AI reduces documentation time through voice recognition and structured data entry. Real-world implementations show dramatic improvements such as documentation dropped from 10–15 minutes to about 1 minute per patient using AI tools.
This shift allows clinicians to focus on patient care instead of paperwork.
• Real-Time Communication and Doctor Nurse Communication Tools
AI-powered platforms strengthen doctor nurse communication tools and enable seamless collaboration. These systems enhance care team coordination systems, ensuring timely interventions.
• Predictive Patient Flow Management
AI analyses patient movement patterns and prevents bottlenecks. Hospitals achieve smoother operations through healthcare workflow automation.
The Role of AI Hospital Management Systems in Hospital Workflow Management
Modern AI hospital management systems integrate all hospital functions into a unified platform.
• Centralised Data and Workflow Integration
Hospitals gain complete visibility into operations. Integrated platforms support interdisciplinary workflow healthcare and eliminate silos.
• End-to-End Healthcare Workflow Optimisation
AI-driven systems automate processes from admission to discharge. These systems improve hospital workflow management and reduce manual effort.
• Real-Time Decision Support for Leaders
Executives access dashboards that provide actionable insights. AI empowers leaders to optimise resources and improve outcomes.
• Scalable Multi-Facility Coordination
Large hospital networks benefit from unified care team coordination systems that ensure consistency across locations.
Also Read – The Impact Of AI On Hospital Management: What You Should Know – Ezovion
How AI Hospital Management Systems Prevent Loss of Clinical Hours
AI eliminates time-consuming tasks that reduce clinical productivity.
| Task | Traditional Time Consumption | AI-Driven Outcome |
| Documentation | High manual effort | Automated via AI |
| Record Retrieval | Time-consuming | Instant access |
| Communication | Delayed | Real-time collaboration |
| Scheduling | Inefficient | Predictive optimisation |
Healthcare organisations that adopt AI healthcare workflow optimisation regain hours previously lost to inefficiencies.
Improving Patient Care Through Healthcare Workflow Optimisation
Effective healthcare workflow optimisation enhances patient outcomes by:
- Reducing waiting times
- Improving care coordination
- Enabling faster diagnosis
- Enhancing patient satisfaction
Hospitals that implement healthcare workflow automation create smoother patient journeys and deliver higher-quality care.
Enhancing Doctor and Nurse Productivity with AI Healthcare Workflow Optimisation
AI transforms clinical workflows by reducing workload and improving efficiency.
- Clinicians spend more time on patient care
- Administrative burden decreases
- Burnout levels reduce
- Job satisfaction improves
Advanced AI workflow assistant healthcare tools support clinicians in real time, enabling better decision-making and coordination.
Also Read – Artificial Intelligence (AI) In Healthcare & Medical Field – Ezovion.
ROI of AI Healthcare Workflow Optimisation for Hospital Workflow Management
Hospital leaders prioritise return on investment. AI-driven systems deliver measurable financial benefits:
- Reduced operational costs
- Improved resource utilisation
- Increased patient throughput
- Enhanced revenue cycles
By implementing AI hospital management systems, hospitals achieve sustainable growth while maintaining care quality.
The Future of Hospital Workflow Management
Healthcare continues to evolve rapidly. Hospitals must transition from reactive systems to predictive ecosystems.
Future trends include:
- Autonomous clinical workflows
- Advanced AI healthcare workflow optimisation
- Fully integrated doctor nurse communication tools
- Intelligent care team coordination systems
Hospitals that embrace innovation will lead the next generation of healthcare delivery.
Also Read – 7 Ways Hospital Management Systems Improve Workflow Efficiency – Ezovion.
Healthcare Workflow Optimisation is a Strategic Imperative
The workflow gap continues to challenge hospitals worldwide. Inefficient systems waste time, increase costs, and reduce care quality. However, AI healthcare workflow optimisation provides a clear path forward. Hospitals that invest in AI hospital management systems, advanced doctor nurse communication tools, and robust healthcare workflow automation will eliminate inefficiencies and unlock new levels of performance.
The question no longer focuses on whether hospitals should adopt AI. The real question asks: how quickly can organisations transform their hospital workflow management to close the gap and deliver better care?





